LAP-BAND System |
|
Gastric Bypass |
|
|
|
Description |
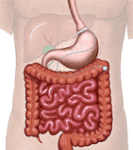
A restrictive procedure, during which an inflatable band is placed around the upper part of the stomach. This creates a smaller stomach pouch, which restricts the amount of food that can be consumed at one time and increases the time it takes for the stomach to empty. As a result, a patient achieves sustained weight loss by limiting food intake, reducing appetite, and slowing digestion |
|
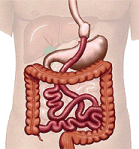
A combination procedure that uses both restrictive and malabsorptive elements. First the stomach is stapled to make a smaller pouch. Then most of the stomach and part of the intestines are bypassed by attaching (usually stapling) a part of the intestine to the small stomach pouch. As a result, a patient cannot eat as much and absorbs fewer nutrients and calories. |
Advantages |
- Lowest mortality rate1
- Least invasive surgical approach
- No stomach stapling or cutting, or intestinal re-routing
- Adjustable
- Reversible
- Lowest operative complication rate
- Low malnutrition risk
|
|
- Rapid initial weight loss
- Minimally invasive approach is common
- Longer clinical experience in the U.S.
- Slightly higher total average weight loss reported than with purely restrictive procedures
|
Disadvantages |
- Slower initial weight loss
- Regular follow-up critical for optimal results
- Requires an implanted medical device
- In some cases, effectiveness can be reduced due to band slippage
- In some cases, the access port may leak and require minor revisional surgery
|
|
- Cutting and stapling of stomach and bowel are required
- More operative complications
- Portion of digestive tract is bypassed, reducing absorption of essential nutrients
- Medical complications due to nutritional deficiencies
- "Dumping syndrome2" can occur
- Non-adjustable
- Extremely difficult to reverse
- Higher mortality rate
|
Results |
Although during the first year after surgery, weight loss with the gastric bypass is greater than with the LAP-BAND® System, surgeons report that at 5 years many LAP-BAND® and gastric bypass patients achieve comparable weight loss (55% for LAP-BAND® and 59% for Gastric Bypass). |
Risks |
Mortality rate: 0.05%
Total complications: 9%
Major complications: 0.2%
Most common include:
- Standard risks associated with major surgery
- Nausea and vomiting
- Band slippage (minor revisional surgery)
- Band erosion (minor revisional surgery)
- Access port problems (minor revisional surgery)
|
|
Mortality rate: 0.5-2%
Total complications: 23%
Major complications: 2.1%
Most common include:
- Standard risks associated with major surgery
- Nausea and vomiting
- Separation of stapled areas (major revisional surgery)
- Leaks from staple lines (major revisional surgery)
- Nutritional deficiencies
|
Costs and Insurance |
Generally speaking, both procedures will be covered by insurance, but check with your employer or your surgeons office for specific information about your policy. |
Recovery Timeline |
- Hospital stay is usually less than 24 hours
- Most patients return to normal activity within 1 week
- Full surgical recovery usually occurs within about 2 weeks
|
|
With a laparoscopic approach:
- Hospital stay is usually 48-72 hours
- Many patients return to normal activity within 2.5 weeks
- Full surgical recovery usually occurs within about 3 weeks
|
1. American Society for Bariatric Surgery, Rationale for the surgical treatment of morbid obesity. American Society for Bariatric Surgery Web site. April 8, 1998. Available at: http://www.asbs.org/html/patients/rationale.html. Accessed April 2006.
2. Ren CJ, Laker S, Weiner M, Hajoseuedhavadi O. . J Am Coll Surg. 2006;202:. Executive summary: Laparoscopic adjustable gastric banding for the treatment of obesity, ASERNIPS 2002.
3. “Dumping syndrome” is a physiological reaction frequently seen following gastric bypass surgery, which is designed to alter anatomy and interrupt normal digestion. Whenever patients eat foods such as sugar and sweets, they may experience symptoms of nausea, flushing and sweating, light-headedness, and watery diarrhea.
4. Fisher B. Obes Surg.2004;14:67-72.